Growing teeth instead of fixing them
For decades, dentistry has largely focused on repairing damage to teeth – filling cavities, capping teeth with crowns, or replacing them with implants. These are effective solutions, certainly, but they address the symptom, not the cause. What if, instead of restoring what’s lost, we could simply grow it back? That’s the promise of tooth regeneration, and it’s rapidly moving from science fiction toward a tangible reality.
Current restorative methods aren’t without their downsides. Costs can be substantial, especially for implants. Procedures are often invasive, and even with the best materials, achieving a completely natural aesthetic result can be challenging. A regenerated tooth, grown from the body’s own cells, could potentially overcome all of these limitations.
The idea isn’t simply to patch things up, but to stimulate the body’s own natural regenerative capabilities. This isn’t about "fake’ teeth; it’s about prompting the formation of actual, living tooth structures – enamel, dentin, pulp, and all. It’s a fundamentally different approach to dental care, and it"s driven by advances in fields like tissue engineering and, crucially, gene therapy.
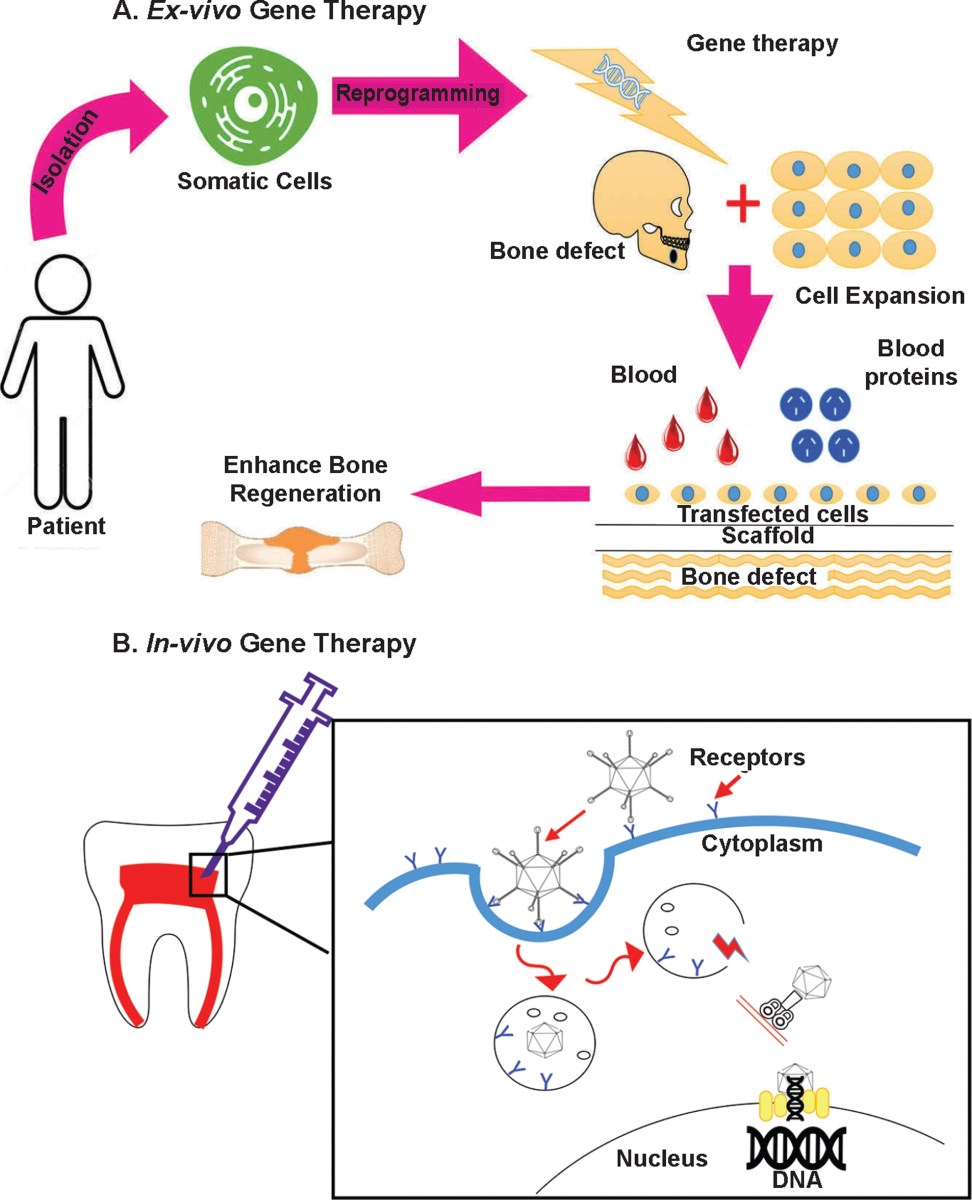
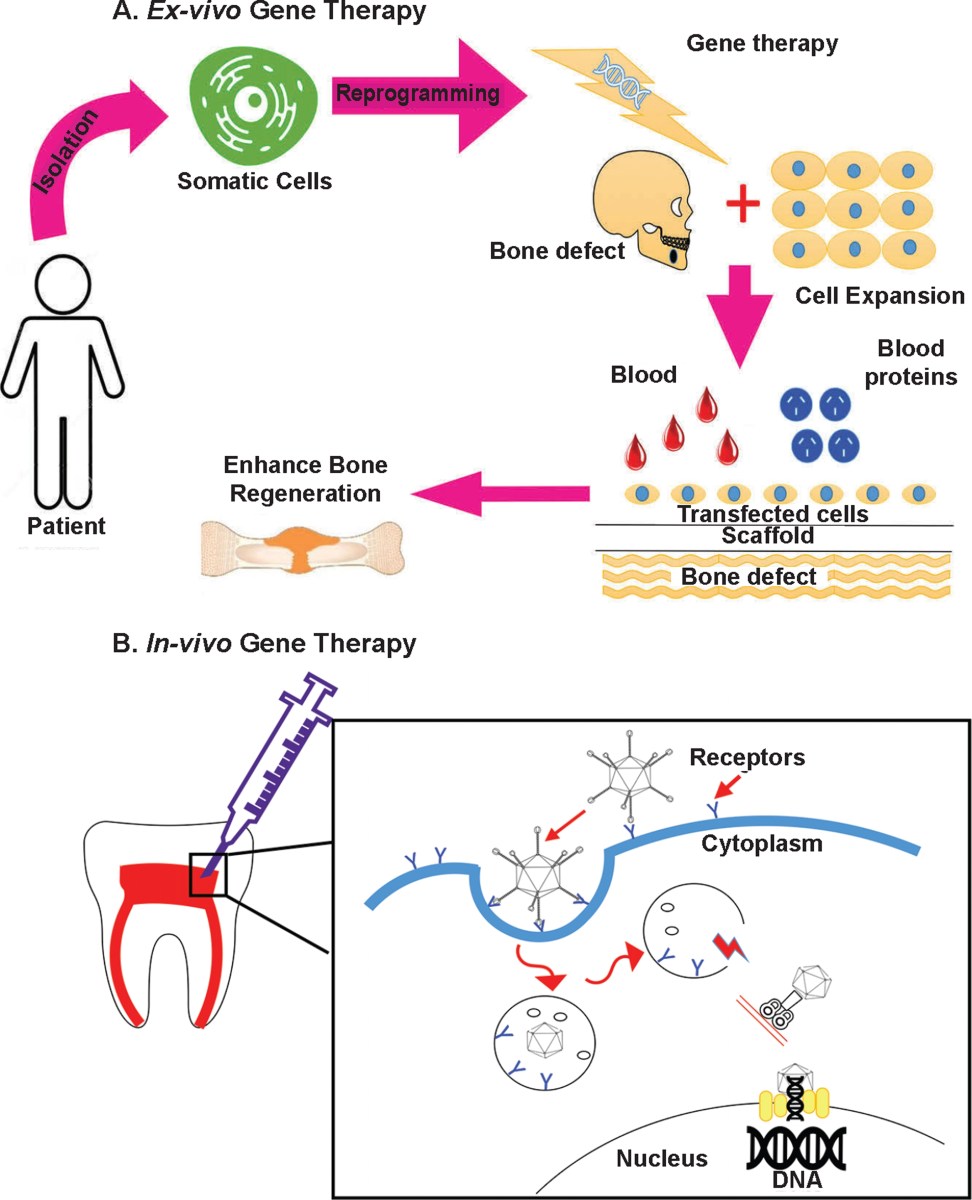
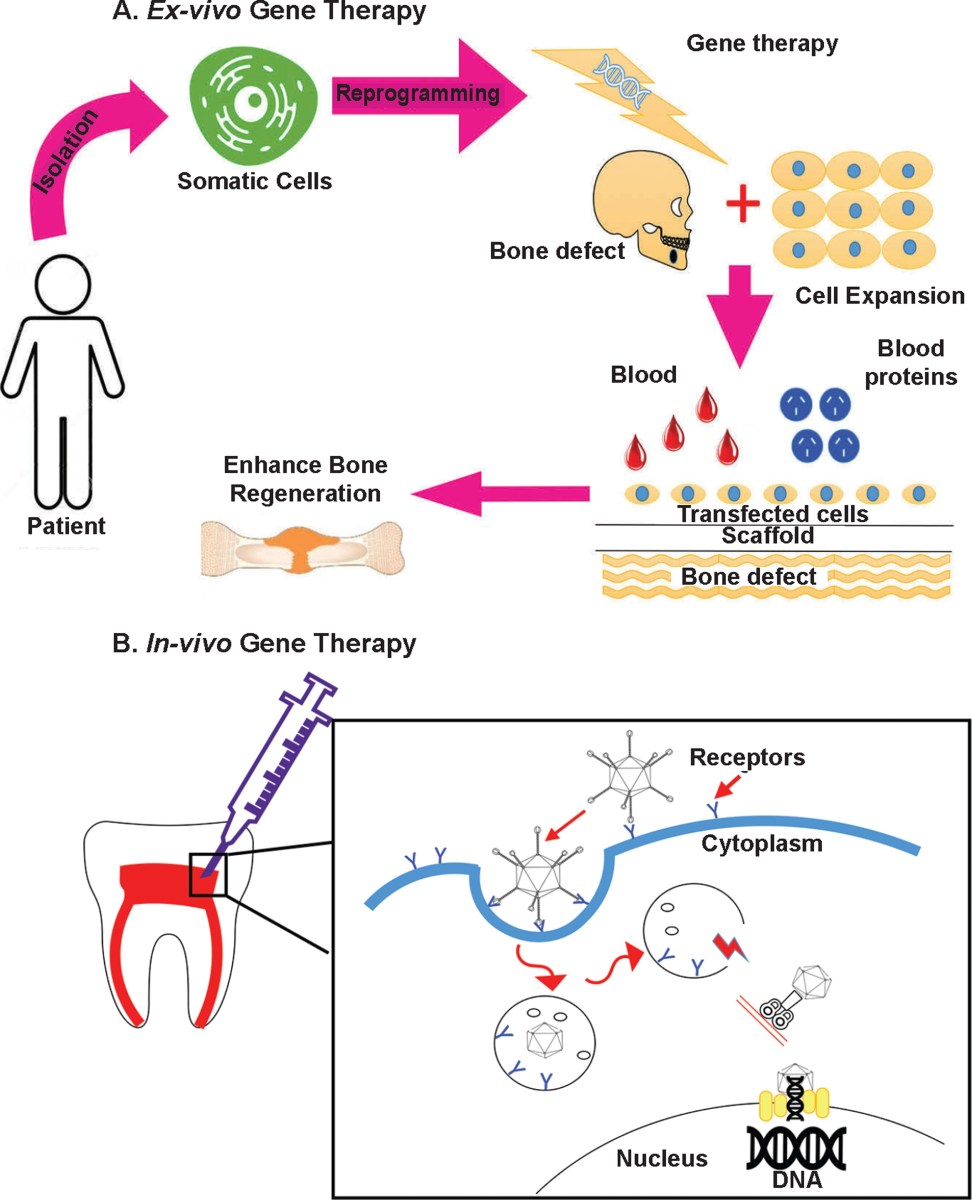
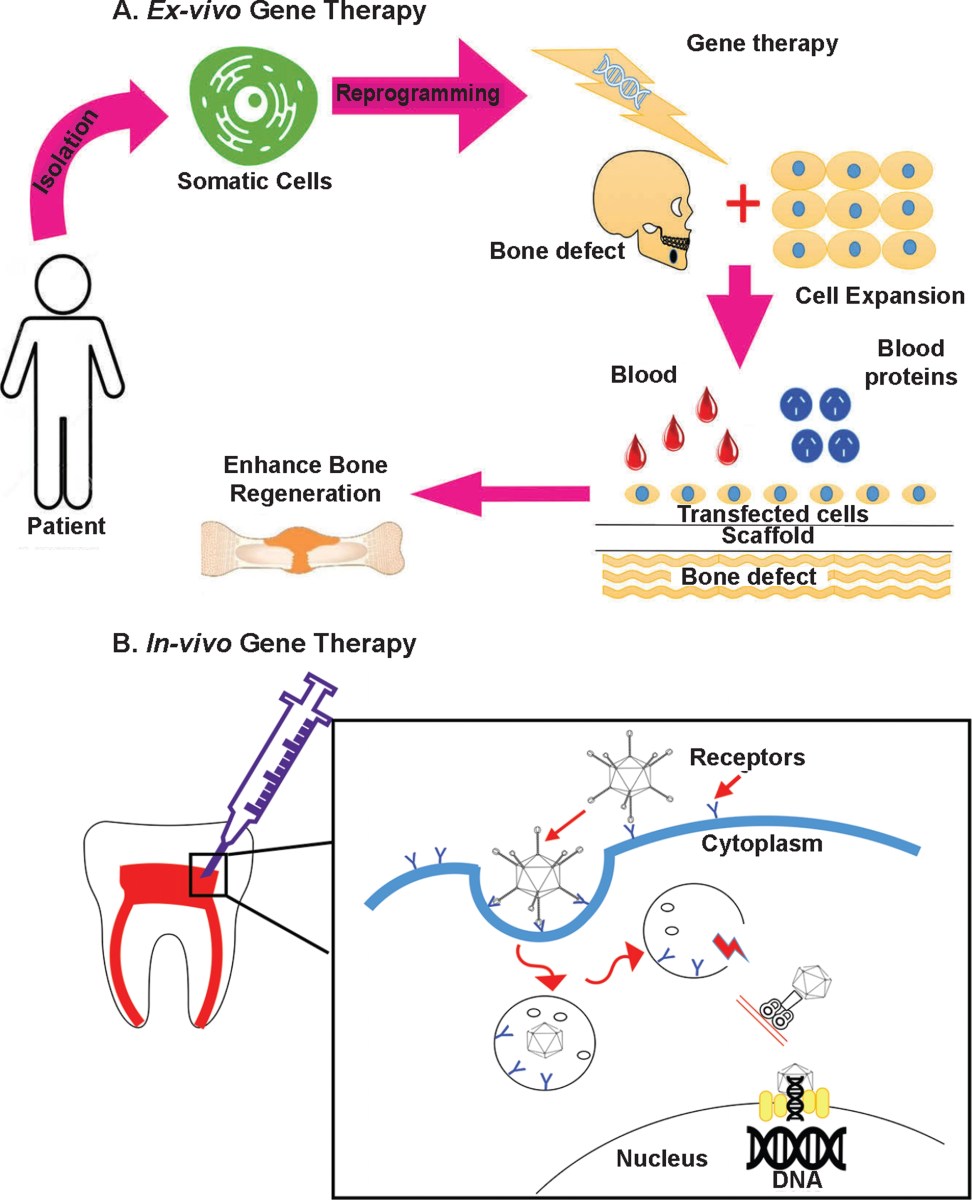
How gene therapy builds enamel
Gene therapy works by putting genetic material into cells to fix or prevent health issues. For teeth, we send instructions to cells to start rebuilding. We aren't changing who you are genetically; we are just giving your cells a temporary manual for building a tooth.
Specific genes are key. Researchers are focusing on genes like Amelogenin, which plays a critical role in enamel formation, and genes involved in dentinogenesis – the creation of dentin, the layer beneath enamel. Other targets include genes that regulate root development and the formation of the dental pulp, which contains the tooth’s nerves and blood vessels. The trick is delivering these genes effectively and safely.
This is where viral vectors come in. Viruses are naturally adept at delivering genetic material into cells. Scientists modify these viruses, removing their harmful components and using them as vehicles to carry therapeutic genes. Adeno-associated viruses (AAVs) are commonly used because they are relatively safe and don’t typically cause illness. However, safety is still a primary concern, and researchers are continually working to refine these vectors and minimize the risk of off-target effects – delivering the gene to the wrong cells.
Breakthroughs in 2026: Key Research Findings
2026 has seen remarkable progress in tooth regeneration research. A study published in Scientific Reports (June 2026) by researchers at the National Institute of Dental and Craniofacial Research (NIDCR) demonstrated complete tooth regeneration in pigs – achieving fully functional molars with healthy enamel, dentin, and periodontal ligament. This built on earlier work with mice, but the larger size and physiological similarity of pigs to humans makes this a significant step forward.
Another breakthrough, reported in the Journal of Dental Research (October 2026), details a new AAV vector with improved targeting specificity, reducing off-target gene delivery by 40% in pre-clinical trials. This vector, developed by a team at the University of California, San Francisco, shows particular promise for treating localized tooth defects.
Human trials, while still in their early stages, are underway. A Phase 1 clinical trial at the University of Tokyo, initiated in early 2026, is evaluating the safety and feasibility of gene therapy for localized enamel defects in children. Preliminary results, presented at the International Association for Dental Research (IADR) conference in July 2026, showed no serious adverse effects and encouraging signs of enamel regeneration. The NIDCR is also funding a multi-center study to assess the long-term efficacy of a similar approach.
Importantly, the ADA’s Clinical Practice Guidelines are beginning to address the ethical considerations of these therapies, emphasizing the need for informed consent and careful patient selection. They released a preliminary statement in November 2026 acknowledging the rapidly evolving field and the importance of evidence-based practice.
- June 2026: NIDCR researchers successfully grew full molars in pigs, including the periodontal ligament.
- October 2026 (Journal of Dental Research): New AAV vector with improved targeting specificity.
- Early 2026 (University of Tokyo): Phase 1 human trial for enamel defects initiated.
Remaining hurdles
Despite the exciting progress, significant challenges remain before gene therapy for tooth regeneration becomes a routine clinical procedure. Off-target effects, while reduced by newer vectors, are still a concern. Ensuring that the therapeutic gene is delivered only to the intended cells is crucial to avoid unintended consequences.
The body’s immune response to viral vectors is another hurdle. The immune system may recognize the vector as foreign and mount an attack, reducing the effectiveness of the therapy. Strategies to suppress the immune response are being investigated, but they must be carefully balanced against the risk of increasing susceptibility to infection.
Long-term stability is also a question. Will the regenerated tooth structures remain healthy and functional for a lifetime? More research is needed to understand the durability of these tissues and to develop strategies to prevent degeneration. Finally, scaling up production of these therapies to meet potential demand will be a major logistical challenge.
Impact on Dental Practice: A Shifting Role
This tech will change how we work. At first, oral surgeons and periodontists will probably handle the injections because the precision required is high. It is a specialized skill set that goes beyond standard drilling and filling.
Over time, as the technology becomes more refined and accessible, it’s possible that general dentists could also be involved, perhaps administering the therapy under the guidance of a specialist. However, a significant shift in dental education and training will be necessary.
The demand for traditional restorative treatments – fillings, crowns, implants – could decrease as regenerative therapies become more widespread. This doesn’t mean these treatments will disappear entirely; they will likely still be needed for cases where regeneration isn’t feasible or for addressing existing damage. But the emphasis will shift from repair to prevention and regeneration.
Ethical considerations are paramount. Dentists will need to be prepared to discuss the risks and benefits of gene therapy with their patients, ensuring they have a clear understanding of the potential outcomes and the limitations of the technology. The ADA is already working on developing guidelines to address these ethical concerns.
Money and management
The financial implications for dental practices are substantial. The initial cost of gene therapy treatments is likely to be high, reflecting the complexity of the procedures and the cost of the therapeutic agents. Insurance coverage will be a critical factor in determining access to these treatments. It’s reasonable to expect a period of uncertainty as insurers grapple with how to classify and reimburse these novel therapies.
Practices may need to invest in new equipment and facilities to support gene therapy procedures. This could include specialized delivery systems, sterile environments, and potentially even on-site gene editing capabilities. The cost of these investments could be significant, particularly for smaller practices.
Patient expectations will undoubtedly change. Patients may become less willing to accept traditional restorative treatments if a regenerative option is available. Dentists will need to be prepared to manage these expectations and to provide patients with realistic assessments of the potential benefits and limitations of each treatment approach.
The shift towards regenerative dentistry could also impact practice marketing and patient communication. Highlighting a practice’s expertise in regenerative therapies could become a key differentiator, attracting patients who are seeking cutting-edge dental care.



No comments yet. Be the first to share your thoughts!